Wellness & You
Main navigation.
- Aetna education
- Healthy all year
- Live well guide
- Benefit spotlight

Related articles

Find local support for healthy living

5 reasons to use your secure member website
Have questions we can help..
Call us at 1-833-570-6670 (TTY: 711) between 8 AM and 8 PM, seven days a week. Or visit AetnaMedicare.com
Free webinar May 9: How to spot and stop a scam. Sign up now.
AARP daily Crossword Puzzle
Hotels with AARP discounts
Life Insurance
AARP Dental Insurance Plans
AARP MEMBERSHIP — $12 FOR YOUR FIRST YEAR WHEN YOU SIGN UP FOR AUTOMATIC RENEWAL
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
- right_container
Work & Jobs
Social Security
AARP en Español
- Membership & Benefits
AARP Rewards
- AARP Rewards %{points}%
Conditions & Treatments
Drugs & Supplements
Health Care & Coverage
Health Benefits

Staying Fit
Your Personalized Guide to Fitness

AARP Hearing Center
Ways To Improve Your Hearing

Brain Health Resources
Tools and Explainers on Brain Health

A Retreat For Those Struggling
Scams & Fraud
Personal Finance
Money Benefits

View and Report Scams in Your Area

AARP Foundation Tax-Aide
Free Tax Preparation Assistance

AARP Money Map
Get Your Finances Back on Track

How to Protect What You Collect
Small Business
Age Discrimination

Flexible Work
Freelance Jobs You Can Do From Home

AARP Skills Builder
Online Courses to Boost Your Career

31 Great Ways to Boost Your Career

ON-DEMAND WEBINARS
Tips to Enhance Your Job Search

Get More out of Your Benefits

When to Start Taking Social Security

10 Top Social Security FAQs

Social Security Benefits Calculator

Medicare Made Easy
Original vs. Medicare Advantage

Enrollment Guide
Step-by-Step Tool for First-Timers

Prescription Drugs
9 Biggest Changes Under New Rx Law

Medicare FAQs
Quick Answers to Your Top Questions
Care at Home
Financial & Legal
Life Balance

LONG-TERM CARE
Understanding Basics of LTC Insurance

State Guides
Assistance and Services in Your Area

Prepare to Care Guides
How to Develop a Caregiving Plan

End of Life
How to Cope With Grief, Loss
Recently Played
Word & Trivia
Atari® & Retro
Members Only
Staying Sharp
Mobile Apps
More About Games

Right Again! Trivia

Right Again! Trivia – Sports

Atari® Video Games

Throwback Thursday Crossword
Travel Tips
Vacation Ideas
Destinations
Travel Benefits

Beach vacation ideas
Vacations for Sun and Fun

Plan Ahead for Tourist Taxes

AARP City Guide
Discover Seattle

25 Ways to Save on Your Vacation
Entertainment & Style
Family & Relationships
Personal Tech
Home & Living
Celebrities
Beauty & Style

TV for Grownups
Best Reality TV Shows for Grownups

Robert De Niro Reflects on His Life

Looking Back
50 World Changers Turning 50

Sex & Dating
Spice Up Your Love Life

Navigate All Kinds of Connections

Life & Home
Couple Creates Their Forever Home

Store Medical Records on Your Phone?

Maximize the Life of Your Phone Battery

Virtual Community Center
Join Free Tech Help Events

Create a Hygge Haven

Soups to Comfort Your Soul

Your Ultimate Guide to Mulching
Driver Safety
Maintenance & Safety
Trends & Technology

AARP Smart Guide
How to Keep Your Car Running

We Need To Talk
Assess Your Loved One's Driving Skills

AARP Smart Driver Course

Building Resilience in Difficult Times

Tips for Finding Your Calm

Weight Loss After 50 Challenge

Cautionary Tales of Today's Biggest Scams

7 Top Podcasts for Armchair Travelers

Jean Chatzky: ‘Closing the Savings Gap’

Quick Digest of Today's Top News

AARP Top Tips for Navigating Life

Get Moving With Our Workout Series
You are now leaving AARP.org and going to a website that is not operated by AARP. A different privacy policy and terms of service will apply.
Go to Series Main Page
Will Medicare cover me if I travel outside the United States?
Kimberly Lankford,
Medicare doesn’t pay for medical services outside the United States or its territories, except in very limited circumstances, including if:
- You experience a medical emergency while traveling between Alaska and another state and a Canadian hospital is closest to your location.
- You face a medical emergency while you’re in the United States or one of its territories, but the nearest hospital is across the border, for example in Canada or Mexico.
- You live in the United States or one of its territories and need hospital care, regardless of whether it’s an emergency, but the nearest hospital is in a foreign country.
- You need medical attention and you’re on a ship within six hours of a U.S. port.
Medicare covers all 50 states and the District of Columbia as well as U.S. territories American Samoa, Guam, the Northern Mariana Islands, Puerto Rico and the U.S. Virgin Islands.

AARP Membership — $12 for your first year when you sign up for Automatic Renewal
What kind of care outside the U.S. will Medicare cover?
In rare situations, Medicare Part A will cover inpatient hospitalization and Medicare Part B will cover emergency ambulance and doctor services immediately before and during your hospital stay.
The same deductibles, copayments and coinsurance apply as for services in the U.S. But coverage is limited: Medicare won’t pay for ambulance or doctor services in the foreign country after your covered hospital stay ends.
If you qualify, the foreign hospital may file a claim with Medicare, but it’s not required to do so. In that case, you may need to submit an itemized bill to Medicare. If you receive care on a cruise ship within six hours of a U.S. port, the attending doctor usually submits the Medicare claim.
Do Medicare supplement policies cover foreign travel?
If you buy a private Medicare supplement policy , better known as Medigap, you may be insured for foreign travel emergencies. Medigap plans C, D, F, G, M and N cover emergency health care while traveling outside of the country. But plans C and F are no longer available to new Medicare beneficiaries; only those eligible for Medicare before 2020 can enroll in plans C and F.
Medigap plans cover foreign travel emergency care that begins in the first 60 days of your trip. They pay 80 percent of the billed charges for specific medically necessary emergency care you receive outside the U.S., but you must first pay a $250 deductible for the year. Medigap’s foreign travel emergency coverage has a lifetime limit of $50,000.

AARP NEWSLETTERS

%{ newsLetterPromoText }%
%{ description }%
Privacy Policy
ARTICLE CONTINUES AFTER ADVERTISEMENT
What other foreign travel emergency coverage is available?
Medicare Advantage. Some private Medicare Advantage plans cover foreign travel emergency care, but here, too, coverage is limited and details vary. Find out more about the Medicare Advantage plans available in your area by using the Medicare Plan Finder .
Travel insurance. While some travel insurance policies cover trip cancellations, others also cover emergency medical care in a foreign country and medical evacuation either to a nearby medical facility or back to the U.S. However, some travel insurance policies exclude preexisting conditions, so find out about exclusions, coverage limits and other details before choosing a policy.
Tricare for Life. If you’re a military retiree, you may have foreign-country health care coverage through Tricare for Life after you enroll in Medicare. Tricare for Life typically covers Medicare’s deductibles, copayments and coinsurance, but it also provides additional benefits, such as health care outside of the U.S. It’s the same foreign travel insurance military retirees and dependents have before enrolling in Medicare. You pay any deductibles and copayments for that coverage.
AARP® Vision Plans from VSP™
Exclusive vision insurance plans designed for members and their families
Keep in mind
If you plan to live abroad or travel back and forth regularly, rather than just vacation out of the country, you can enroll in Medicare. But you’ll forgo coverage while you’re away and still have to pay the monthly Part B premiums , typically $174.70 a month in 2024. You’ll also have to pay Part A premiums if you or your spouse haven’t paid Medicare taxes for at least 10 years.
If you decide to wait to enroll in Medicare until after you return to the United States, you may have to pay a late enrollment penalty . If you work abroad and receive health insurance from your employer, live in a country with a national health system or volunteer and have health coverage through a sponsor organization, you may have some exemptions.
This includes eligibility for an eight-month special enrollment period after you stop working or lose your insurance; six months if you’re volunteering. It’s a good idea to research your options before making any decisions about health care insurance while traveling.
Return to Medicare Q&A main page
Kimberly Lankford is a contributing writer who covers Medicare and personal finance. She wrote about insurance, Medicare, retirement and taxes for more than 20 years at Kiplinger’s Personal Finance and has written for The Washington Post and Boston Globe . She received the personal finance Best in Business award from the Society of American Business Editors and Writers and the New York State Society of CPAs’ excellence in financial journalism award for her guide to Medicare.
Discover AARP Members Only Access
Already a Member? Login

More From AARP

10 Things Medicare Doesn’t Cover
You’ll need to plan ahead to pay for some common medical expenses

Where Can I Find Answers to My Medicare Questions?
We have 5 resources for you to check out, including AARP

How Are Medigap and Medicare Advantage Plans Different?
AARP Value & Member Benefits

Learn, earn and redeem points for rewards with our free loyalty program

AARP® Dental Insurance Plan administered by Delta Dental Insurance Company
Dental insurance plans for members and their families

The National Hearing Test
Members can take a free hearing test by phone

AARP® Staying Sharp®
Activities, recipes, challenges and more with full access to AARP Staying Sharp®
SAVE MONEY WITH THESE LIMITED-TIME OFFERS
Traveling with Medicare: What You Need to Know
Emergencies are unexpected, no matter where you are. Know what to expect from Medicare when traveling in and out of the country.
Written by Alex Rivera • June 15, 2022 • 4 min read
Medicare and Traveling: The Basics
Before you book your next travel destination, ensure you’re prepared for any unexpected medical emergencies. The type of Medicare plan you use, as well as where you travel, will affect your coverage. For example, because Original Medicare is federal health insurance, you can expect coverage across the 50 states and U.S. territories, including the District of Columbia, Puerto Rico, the Virgin Islands, Guam, American Samoa, and the Northern Mariana Islands. Medicare Advantage plans , on the other hand, serve specific areas. Your vacation destination might be outside of that service area, so be sure to understand where your Advantage plan starts and ends or you might find yourself knee-deep in medical bills. Outside the country, Medicare coverage is limited for both Original Medicare and Medicare Advantage plans. Advantage plans are required to cover emergency and urgent care in the U.S. as long as you’re in the service area of the plan, but don’t have that same requirement outside the country. Medigap plans may cover services not included in your current Medicare plans. Read on to learn when you’re covered and when you’re not as you travel inside and outside the country.

Medicare coverage when traveling domestically
Medicare covers services from sea to shining sea—and beyond. Not only does Medicare take care of your medical business in all 50 U.S. states, it assumes coverage in U.S. territories as well. Whether you’re sailing off the beaches of Puerto Rico, learning the haka on the islands of American Samoa, or visiting the Capitol in the District of Columbia, Medicare has you covered.
Domestic travel isn’t complicated for Original Medicare, though Medicare Advantage may have some limitations. Every Medicare Advantage plan has specific service areas and health insurance networks. Only certain locations, doctors, and hospitals are covered under a Medicare Advantage plan. Because each plan is different, call your provider ahead of time to ensure that your Medicare Advantage plan provides coverage in your travel destination. Medigap plans cover expenses not included in your Advantage or Original Medicare plans. Like Medicare, Medigap offers coverage just about anywhere in the United States. It will help supplement any copayments, coinsurances, or deductibles that your Medicare plan doesn’t cover. Some Medigap plans also include prescription drug coverage, similar to some Medicare Advantage plans.
Find the plan that best suits your domestic travel needs.
- Original Medicare: When traveling in the U.S., Original Medicare coverage is comprehensive. As long as you’re in one of the states or U.S. territories, you can be sure that Original Medicare will cover at least part of it.
- Medicare Advantage: Although some Medicare Advantage plans have limitations regarding coverage, they still can cover quite a bit of real estate. Depending on the plan you choose, you may or may not have coverage at certain hospitals or with certain physicians. Make sure you contact your provider to see where your Medicare Advantage plan is accepted.
- Medigap: Medigap provides supplemental coverage for services that your Original Medicare or Medicare Advantage plans don’t cover. Like Original Medicare, there aren’t any restrictions that would stop Medigap from filling in the gap when traveling within the U.S.
- Part D Prescription Coverage: You can pair your Medicare Advantage plan or Medigap plan with a prescription drug plan. When traveling domestically, coverage is relatively straightforward—just ensure that your plan is accepted where you’re going.

Medicare coverage when traveling internationally
If you’re looking to travel North or South of the border or across the pond, Medicare can get complicated. Original Medicare won’t pay for most supplies and services outside the United States. There are very specific exemptions to this rule , leaving little room for coverage in a foreign place.
Be sure to research Medicare Advantage providers during AEP, as some Advantage plans offer international coverage. Not all Medicare Advantage plans are created equal, but Aetna , for example, offers some of the best international coverage out there. From emergency care to urgent care, Aetna’s Medicare Advantage plans have you in mind when you travel abroad.
Unfortunately, prescription drug coverage is also not available outside of the U.S., even when paired with a Medicare Advantage plan. Some Medigap plans help cover services overseas , but you must meet particular prerequisites to receive additional help from Medigap in a foreign country. Medigap coverage may depend upon how long you have been in the foreign country, the type of service you are receiving, and the payment of a $250 deductible.
Medicare’s lack of international coverage may seem dire, but all is not lost when it comes to health coverage overseas. Although separate from Medicare, international travel insurance pays for emergency and routine medical services outside the U.S. Each travel insurance plan is different, so plan ahead based on potential needs.
International travel is more enjoyable when you know you’re covered. Find the plan that puts your health first.
- Original Medicare: In most situations, Medicare won’t pay for health care or supplies you get outside the U.S., with few exceptions.
- Medicare Advantage: Unlike Original Medicare, there are Medicare Advantage plans that offer comprehensive international coverage. Take a closer look at Aetna Medicare Advantage plans for example.
- Medigap: Medigap covers foreign travel emergency care if it begins during the first 60 days of your trip. Medigap also pays 80% of the billed charges for certain medically necessary emergency care outside the U.S. after you meet a $250 deductible for the year.
- Part D Prescription Coverage: If you purchase prescription drugs outside of the U.S., do not expect Medicare drug plans to cover them. You’ll need to get travel insurance or Medigap* to potentially help pay those expenses.
* Medigap will only potentially cover 80% of medically-necessary prescription drugs that are administered in a hospital during a medically-necessary stay.
Quick Medicare & Travel Guide
The following chart shows you which Medicare plans cover what services both domestically and internationally. Remember: if you have questions or need extra help enrolling in a new plan with better travel coverage, call 833-716-0673 to speak with a licensed Medicare agent.
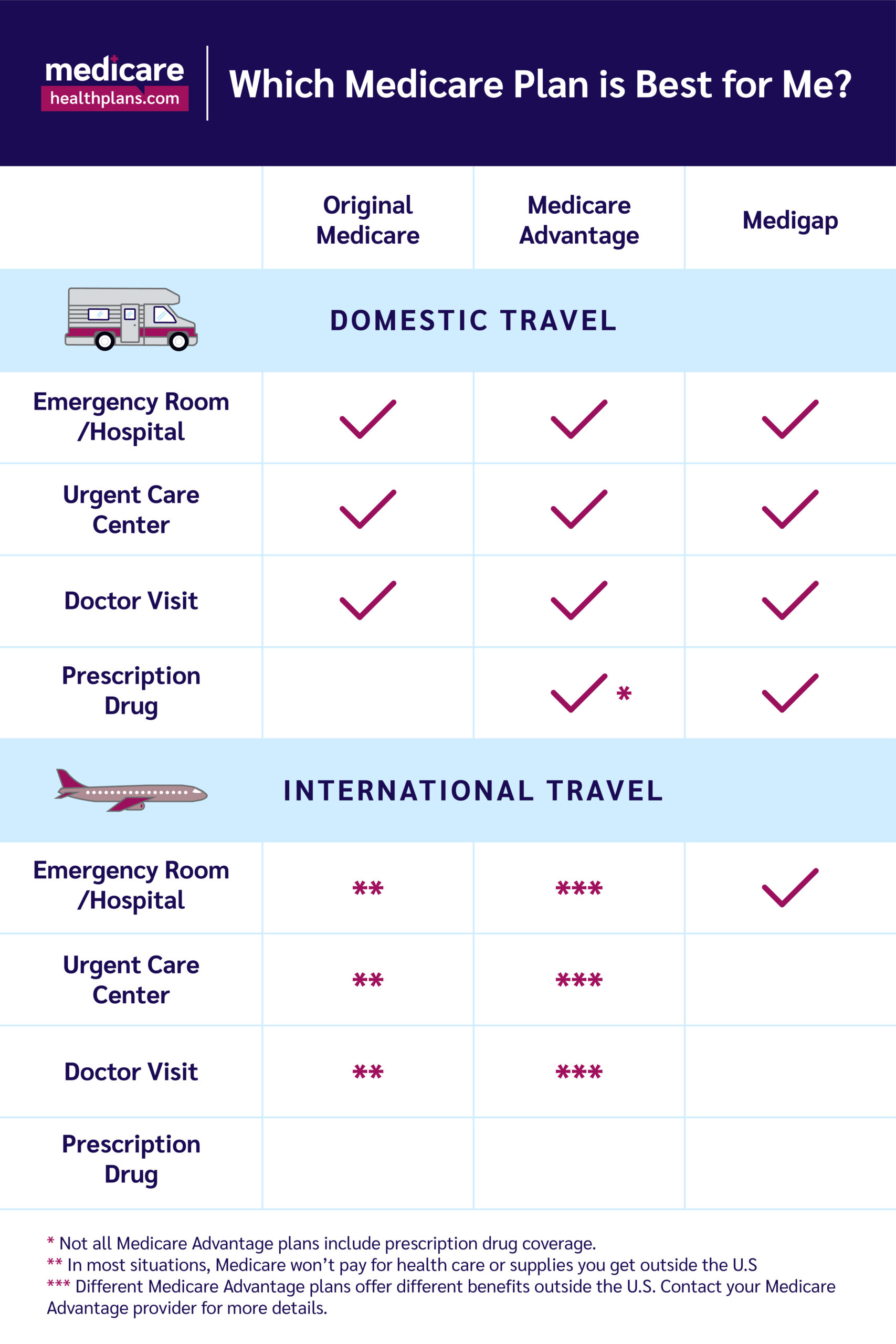
Additional Resources:
Recent articles.
Annual Enrollment Period (AEP)
6 Common Medicare Mistakes and How to Avoid Them
Alex Rivera
November 16, 2022 • 4 min read
Social Media
The Top Social Media Influencers Over 65
October 12, 2022 • 3 min read
7 Ways to Prepare for the 2022 Annual Enrollment Period
October 10, 2022 • 3 min read
Back to top
Travel outside the U.S.
Medicare usually doesn’t cover health care while you’re traveling outside the U.S. There are some exceptions, including some cases where Medicare Part B (Medical Insurance) may pay for services that you get on board a ship within the territorial waters adjoining the land areas of the U.S. However, Medicare won't pay for health care services you get when a ship is more than 6 hours away from a U.S. port.
Medicare may pay for inpatient hospital , doctor , and ambulance services you get in a foreign country in these rare cases:
- You're in the U.S. when a medical emergency occurs, and the foreign hospital is closer than the nearest U.S. hospital that can treat your medical condition.
- You're traveling through Canada without unreasonable delay by the most direct route between Alaska and another U.S state when a medical emergency occurs, and the Canadian hospital is closer than the nearest U.S. hospital that can treat the emergency.
- You live in the U.S. and the foreign hospital is closer to your home than the nearest U.S. hospital that can treat your medical condition, regardless of whether an emergency exists.
Medicare may cover medically necessary ambulance transportation to a foreign hospital only with admission for medically necessary covered inpatient hospital services.
Medicare drug coverage (Part D) covers all vaccines that the Advisory Committee on Immunization Practices (ACIP) recommends, including certain vaccines you might need to get before you travel outside the U.S. (like yellow fever, chikungunya, and Japanese encephalitis). Your Part D plan won't charge you a copayment or apply a deductible for vaccines ACIP recommends. Contact your Medicare drug plan for details and talk to your provider about which ones are right for you.
Your costs in Original Medicare
You pay 100% of the costs, in most cases. In the situations described above, you pay the part of the charge you would normally pay for covered services. This includes any medically necessary doctor and ambulance services you get in a foreign country as a part of a covered inpatient hospital stay. You also pay the coinsurance, copayments, and deductibles you'd normally pay if got these same services or supplies inside the U.S.
In the situations above, Medicare pays only for services covered under Original Medicare : Medicare Part A (Hospital Insurance) covers hospital care (care you get when you've been formally admitted with a doctor's order to the foreign hospital as an inpatient).
- Medicare didn't cover your hospital stay.
- You got ambulance and doctor services outside the hospital after your covered hospital stay ended.
Foreign hospitals aren’t required to file Medicare claims for your travel medical costs. You need to submit an itemized bill to Medicare for your doctor, inpatient, and ambulance services if both of these apply:
- You're admitted to a foreign hospital under one of the situations above
- The foreign hospital doesn't submit Medicare claims for you
To find out how much your test, item, or service will cost, talk to your doctor or health care provider. The specific amount you’ll owe may depend on several things, like:
- Other insurance you may have
- How much your doctor charges
- If your doctor accepts assignment
- The type of facility
- Where you get your test, item, or service
Things to know
The 50 states, the District of Columbia, Puerto Rico, the U.S. Virgin Islands, Guam, the Northern Mariana Islands, and American Samoa are considered part of the U.S. Anywhere else is considered outside the U.S.
Medicare drug plans don't cover prescription drugs you buy outside the U.S.
Medicare supplement insurance (Medigap) policies may cover emergency care when you travel outside the U.S.
Because Medicare has limited travel medical coverage outside the U.S., you may choose to buy a travel insurance policy to get more coverage. An insurance agent or travel agent can give you more information about the cost of travel medical insurance. Travel insurance doesn’t necessarily include health insurance, so it’s important to read the conditions or restrictions carefully.
Related resources
- Medicare & You: traveling abroad (video)
Is my test, item, or service covered?
About Aetna
- News & analysis
Initiatives
Health section, international health insurance for individuals.
Enjoy peace of mind wherever you travel with global medical coverage.
We have over 30 years experience in international health insurance. And more than 500,000 members trust us with their care worldwide. We offer:
- Medical insurance
- Dental insurance
- Multiple plan options
- Both short-term and long-term business travel coverage
Visit Aetna International
Designed to help expats find first-class international medical coverage, this type of plan offers a wide range of options to fit a busy lifestyle.
Choose this plan if you:
- Do not use health care or have health insurance in the U.S.
- Want plans that cover doctor visits as well as hospital stays
- Need a maximum per person coverage up to $1.6 million per year
International health insurance for US citizens
This style of coverage gives you access to the highest level of health care and services, regardless of your location.
This insurance plan offers you:
- Worldwide coverage
- 24-hour member support team
- Generous annual maximum coverage
- Emergency medical evacuation
- Coverage for maternity, dental and wellness check-ups
International health insurance for non-US citizens
Legal notices
Aetna is the brand name used for products and services provided by one or more of the Aetna group of companies, including Aetna Life Insurance Company and its affiliates (Aetna).
Health benefits and health insurance plans contain exclusions and limitations.
See all legal notices
Also of interest:
You are now being directed to the AMA site
Links to various non-Aetna sites are provided for your convenience only. Aetna Inc. and its affiliated companies are not responsible or liable for the content, accuracy or privacy practices of linked sites, or for products or services described on these sites.
You are now being directed to the Give an Hour site
Links to various non-Aetna sites are provided for your convenience only. Aetna Inc. and its affiliated companies are not responsible or liable for the content, accuracy or privacy practices of linked sites, or for products or services described on these sites.
You are now being directed to the CVS Pharmacy® site
You are now being directed to the cdc site.
Links to various non-Aetna sites are provided for your convenience only. Aetna Inc. and its its affiliated companies are not responsible or liable for the content, accuracy or privacy practices of linked sites, or for products or services described on these sites.

Aetna® is proud to be part of the CVS Health family.
You are now being directed to the CVS Health site.
You are now being directed to the Apple.com COVID-19 Screening Tool
Links to various non-Aetna sites are provided for your convenience only. Aetna Inc. and its affiliated companies are not responsible or liable for the content, accuracy, or privacy practices of linked sites, or for products or services described on these sites.
You are now being directed to the US Department of Health and Human Services site
You are now being directed to the cvs health covid-19 testing site, you are now being directed to the fight is in us site.
Links to various non-Aetna sites are provided for your convenience only. Aetna Inc. and its affiliated companies are not responsible or liable for the content, accuracy, or privacy practices of linked sites, or for products or services described on these sites.
You are now leaving the Aetna® website
Please log in to your secure account to get what you need.
You are now leaving the Aetna Medicare website.
The information you will be accessing is provided by another organization or vendor. If you do not intend to leave our site, close this message.
Get a link to download the app
Just enter your mobile number and we’ll text you a link to download the Aetna Health℠ app from the App Store or on Google Play.
Message and data rates may apply*
This search uses the five-tier version of this plan
Each main plan type has more than one subtype. Some subtypes have five tiers of coverage. Others have four tiers, three tiers or two tiers. This search will use the five-tier subtype. It will show you whether a drug is covered or not covered, but the tier information may not be the same as it is for your specific plan. Do you want to continue?
Applied Behavior Analysis Medical Necessity Guide
By clicking on “I Accept”, I acknowledge and accept that:
The Applied Behavior Analysis (ABA) Medical Necessity Guide helps determine appropriate (medically necessary) levels and types of care for patients in need of evaluation and treatment for behavioral health conditions. The ABA Medical Necessity Guide does not constitute medical advice. Treating providers are solely responsible for medical advice and treatment of members. Members should discuss any matters related to their coverage or condition with their treating provider.
Each benefit plan defines which services are covered, which are excluded, and which are subject to dollar caps or other limits. Members and their providers will need to consult the member's benefit plan to determine if there are any exclusions or other benefit limitations applicable to this service or supply.
The conclusion that a particular service or supply is medically necessary does not constitute a representation or warranty that this service or supply is covered (i.e., will be paid for by Aetna) for a particular member. The member's benefit plan determines coverage. Some plans exclude coverage for services or supplies that Aetna considers medically necessary.
Please note also that the ABA Medical Necessity Guide may be updated and are, therefore, subject to change.
Medical necessity determinations in connection with coverage decisions are made on a case-by-case basis. In the event that a member disagrees with a coverage determination, member may be eligible for the right to an internal appeal and/or an independent external appeal in accordance with applicable federal or state law.
Aetna® is proud to be part of the CVS® family.
You are now being directed to CVS Caremark ® site.
ASAM Terms and conditions
By clicking on “I accept”, I acknowledge and accept that:
Licensee's use and interpretation of the American Society of Addiction Medicine’s ASAM Criteria for Addictive, Substance-Related, and Co-Occurring Conditions does not imply that the American Society of Addiction Medicine has either participated in or concurs with the disposition of a claim for benefits.
This excerpt is provided for use in connection with the review of a claim for benefits and may not be reproduced or used for any other purpose.
Copyright 2015 by the American Society of Addiction Medicine. Reprinted with permission. No third party may copy this document in whole or in part in any format or medium without the prior written consent of ASAM.
Precertification lists
Should the following terms and conditions be acceptable to you, please indicate your agreement and acceptance by selecting the button below labeled "I Accept".
- The term precertification here means the utilization review process to determine whether the requested service, procedure, prescription drug or medical device meets the company's clinical criteria for coverage. It does not mean precertification as defined by Texas law, as a reliable representation of payment of care or services to fully insured HMO and PPO members.
- Applies to: Aetna Choice ® POS, Aetna Choice POS II, Aetna Medicare ℠ Plan (PPO), Aetna Medicare Plan (HMO), all Aetna HealthFund ® products, Aetna Health Network Only ℠ , Aetna Health Network Option ℠ , Aetna Open Access ® Elect Choice ® , Aetna Open Access HMO, Aetna Open Access Managed Choice ® , Open Access Aetna Select ℠ , Elect Choice, HMO, Managed Choice POS, Open Choice ® , Quality Point-of-Service ® (QPOS ® ), and Aetna Select ℠ benefits plans and all products that may include the Aexcel ® , Choose and Save ℠ , Aetna Performance Network or Savings Plus networks. Not all plans are offered in all service areas.
- All services deemed "never effective" are excluded from coverage. Aetna defines a service as "never effective" when it is not recognized according to professional standards of safety and effectiveness in the United States for diagnosis, care or treatment. Visit the secure website, available through www.aetna.com, for more information. Click on "Claims," "CPT/HCPCS Coding Tool," "Clinical Policy Code Search."
- The five character codes included in the Aetna Precertification Code Search Tool are obtained from Current Procedural Terminology (CPT ® ), copyright 2023 by the American Medical Association (AMA). CPT is developed by the AMA as a listing of descriptive terms and five character identifying codes and modifiers for reporting medical services and procedures performed by physicians.
- The responsibility for the content of Aetna Precertification Code Search Tool is with Aetna and no endorsement by the AMA is intended or should be implied. The AMA disclaims responsibility for any consequences or liability attributable or related to any use, nonuse or interpretation of information contained in Aetna Precertification Code Search Tool. No fee schedules, basic unit values, relative value guides, conversion factors or scales are included in any part of CPT. Any use of CPT outside of Aetna Precertification Code Search Tool should refer to the most Current Procedural Terminology which contains the complete and most current listing of CPT codes and descriptive terms. Applicable FARS/DFARS apply.
LICENSE FOR USE OF CURRENT PROCEDURAL TERMINOLOGY, FOURTH EDITION ("CPT ® ")
- CPT only Copyright 2023 American Medical Association. All Rights Reserved. CPT is a registered trademark of the American Medical Association. You, your employees and agents are authorized to use CPT only as contained in Aetna Precertification Code Search Tool solely for your own personal use in directly participating in health care programs administered by Aetna, Inc. You acknowledge that AMA holds all copyright, trademark and other rights in CPT. Any use not authorized herein is prohibited, including by way of illustration and not by way of limitation, making copies of CPT for resale and/or license, transferring copies of CPT to any party not bound by this agreement, creating any modified or derivative work of CPT, or making any commercial use of CPT. License to sue CPT for any use not authorized herein must be obtained through the American Medical Association, CPT Intellectual Property Services, 515 N. State Street, Chicago, Illinois 60610. Applications are available at the American Medical Association Web site, www.ama-assn.org/go/cpt.
U.S. Government Rights
This product includes CPT which is commercial technical data and/or computer data bases and/or commercial computer software and/or commercial computer software documentation, as applicable which were developed exclusively at private expense by the American Medical Association, 515 North State Street, Chicago, Illinois, 60610. U.S. Government rights to use, modify, reproduce, release, perform, display, or disclose these technical data and/or computer data bases and/or computer software and/or computer software documentation are subject to the limited rights restrictions of DFARS 252.227-7015(b)(2) (June 1995) and/or subject to the restrictions of DFARS 227.7202-1(a) (June 1995) and DFARS 227.7202-3(a) (June 1995), as applicable for U.S. Department of Defense procurements and the limited rights restrictions of FAR 52.227-14 (June 1987) and/or subject to the restricted rights provisions of FAR 52.227-14 (June 1987) and FAR 52.227-19 (June 1987), as applicable, and any applicable agency FAR Supplements, for non-Department of Defense Federal procurements.
Disclaimer of Warranties and Liabilities.
CPT is provided "as is" without warranty of any kind, either expressed or implied, including but not limited to the implied warranties of merchantability and fitness for a particular purpose. No fee schedules, basic unit, relative values or related listings are included in CPT. The American Medical Association (AMA) does not directly or indirectly practice medicine or dispense medical services. The responsibility for the content of this product is with Aetna, Inc. and no endorsement by the AMA is intended or implied. The AMA disclaims responsibility for any consequences or liability attributable to or related to any use, non-use, or interpretation of information contained or not contained in this product.
This Agreement will terminate upon notice if you violate its terms. The AMA is a third party beneficiary to this Agreement.
Should the foregoing terms and conditions be acceptable to you, please indicate your agreement and acceptance by selecting the button labeled "I Accept".
The information contained on this website and the products outlined here may not reflect product design or product availability in Arizona. Therefore, Arizona residents, members, employers and brokers must contact Aetna directly or their employers for information regarding Aetna products and services.
This information is neither an offer of coverage nor medical advice. It is only a partial, general description of plan or program benefits and does not constitute a contract. In case of a conflict between your plan documents and this information, the plan documents will govern.
Dental clinical policy bulletins
- Aetna Dental Clinical Policy Bulletins (DCPBs) are developed to assist in administering plan benefits and do not constitute dental advice. Treating providers are solely responsible for dental advice and treatment of members. Members should discuss any Dental Clinical Policy Bulletin (DCPB) related to their coverage or condition with their treating provider.
- While the Dental Clinical Policy Bulletins (DCPBs) are developed to assist in administering plan benefits, they do not constitute a description of plan benefits. The Dental Clinical Policy Bulletins (DCPBs) describe Aetna's current determinations of whether certain services or supplies are medically necessary, based upon a review of available clinical information. Each benefit plan defines which services are covered, which are excluded, and which are subject to dollar caps or other limits. Members and their providers will need to consult the member's benefit plan to determine if there are any exclusions or other benefit limitations applicable to this service or supply. Aetna's conclusion that a particular service or supply is medically necessary does not constitute a representation or warranty that this service or supply is covered (i.e., will be paid for by Aetna). Your benefits plan determines coverage. Some plans exclude coverage for services or supplies that Aetna considers medically necessary. If there is a discrepancy between this policy and a member's plan of benefits, the benefits plan will govern. In addition, coverage may be mandated by applicable legal requirements of a State or the Federal government.
- Please note also that Dental Clinical Policy Bulletins (DCPBs) are regularly updated and are therefore subject to change.
- Since Dental Clinical Policy Bulletins (DCPBs) can be highly technical and are designed to be used by our professional staff in making clinical determinations in connection with coverage decisions, members should review these Bulletins with their providers so they may fully understand our policies.
- Under certain plans, if more than one service can be used to treat a covered person's dental condition, Aetna may decide to authorize coverage only for a less costly covered service provided that certain terms are met.
Medical clinical policy bulletins
- Aetna Clinical Policy Bulletins (CPBs) are developed to assist in administering plan benefits and do not constitute medical advice. Treating providers are solely responsible for medical advice and treatment of members. Members should discuss any Clinical Policy Bulletin (CPB) related to their coverage or condition with their treating provider.
- While the Clinical Policy Bulletins (CPBs) are developed to assist in administering plan benefits, they do not constitute a description of plan benefits. The Clinical Policy Bulletins (CPBs) express Aetna's determination of whether certain services or supplies are medically necessary, experimental and investigational, or cosmetic. Aetna has reached these conclusions based upon a review of currently available clinical information (including clinical outcome studies in the peer-reviewed published medical literature, regulatory status of the technology, evidence-based guidelines of public health and health research agencies, evidence-based guidelines and positions of leading national health professional organizations, views of physicians practicing in relevant clinical areas, and other relevant factors).
- Aetna makes no representations and accepts no liability with respect to the content of any external information cited or relied upon in the Clinical Policy Bulletins (CPBs). The discussion, analysis, conclusions and positions reflected in the Clinical Policy Bulletins (CPBs), including any reference to a specific provider, product, process or service by name, trademark, manufacturer, constitute Aetna's opinion and are made without any intent to defame. Aetna expressly reserves the right to revise these conclusions as clinical information changes, and welcomes further relevant information including correction of any factual error.
- CPBs include references to standard HIPAA compliant code sets to assist with search functions and to facilitate billing and payment for covered services. New and revised codes are added to the CPBs as they are updated. When billing, you must use the most appropriate code as of the effective date of the submission. Unlisted, unspecified and nonspecific codes should be avoided.
- Each benefit plan defines which services are covered, which are excluded, and which are subject to dollar caps or other limits. Members and their providers will need to consult the member's benefit plan to determine if there are any exclusions or other benefit limitations applicable to this service or supply. The conclusion that a particular service or supply is medically necessary does not constitute a representation or warranty that this service or supply is covered (i.e., will be paid for by Aetna) for a particular member. The member's benefit plan determines coverage. Some plans exclude coverage for services or supplies that Aetna considers medically necessary. If there is a discrepancy between a Clinical Policy Bulletin (CPB) and a member's plan of benefits, the benefits plan will govern.
- In addition, coverage may be mandated by applicable legal requirements of a State, the Federal government or CMS for Medicare and Medicaid members.
See CMS's Medicare Coverage Center
- Please note also that Clinical Policy Bulletins (CPBs) are regularly updated and are therefore subject to change.
- Since Clinical Policy Bulletins (CPBs) can be highly technical and are designed to be used by our professional staff in making clinical determinations in connection with coverage decisions, members should review these Bulletins with their providers so they may fully understand our policies.
- While Clinical Policy Bulletins (CPBs) define Aetna's clinical policy, medical necessity determinations in connection with coverage decisions are made on a case by case basis. In the event that a member disagrees with a coverage determination, Aetna provides its members with the right to appeal the decision. In addition, a member may have an opportunity for an independent external review of coverage denials based on medical necessity or regarding the experimental and investigational status when the service or supply in question for which the member is financially responsible is $500 or greater. However, applicable state mandates will take precedence with respect to fully insured plans and self-funded non-ERISA (e.g., government, school boards, church) plans.
See Aetna's External Review Program
- The five character codes included in the Aetna Clinical Policy Bulletins (CPBs) are obtained from Current Procedural Terminology (CPT®), copyright 2015 by the American Medical Association (AMA). CPT is developed by the AMA as a listing of descriptive terms and five character identifying codes and modifiers for reporting medical services and procedures performed by physicians.
- The responsibility for the content of Aetna Clinical Policy Bulletins (CPBs) is with Aetna and no endorsement by the AMA is intended or should be implied. The AMA disclaims responsibility for any consequences or liability attributable or related to any use, nonuse or interpretation of information contained in Aetna Clinical Policy Bulletins (CPBs). No fee schedules, basic unit values, relative value guides, conversion factors or scales are included in any part of CPT. Any use of CPT outside of Aetna Clinical Policy Bulletins (CPBs) should refer to the most current Current Procedural Terminology which contains the complete and most current listing of CPT codes and descriptive terms. Applicable FARS/DFARS apply.
LICENSE FOR USE OF CURRENT PROCEDURAL TERMINOLOGY, FOURTH EDITION ("CPT®")
CPT only copyright 2015 American Medical Association. All Rights Reserved. CPT is a registered trademark of the American Medical Association.
You, your employees and agents are authorized to use CPT only as contained in Aetna Clinical Policy Bulletins (CPBs) solely for your own personal use in directly participating in healthcare programs administered by Aetna, Inc. You acknowledge that AMA holds all copyright, trademark and other rights in CPT.
Any use not authorized herein is prohibited, including by way of illustration and not by way of limitation, making copies of CPT for resale and/or license, transferring copies of CPT to any party not bound by this agreement, creating any modified or derivative work of CPT, or making any commercial use of CPT. License to use CPT for any use not authorized herein must be obtained through the American Medical Association, CPT Intellectual Property Services, 515 N. State Street, Chicago, Illinois 60610. Applications are available at the American Medical Association Web site, www.ama-assn.org/go/cpt.
Go to the American Medical Association Web site
You are now leaving the Aetna® website.
We're working with 3Won to process your request for participation. Please select "Continue to ProVault to begin the contracting and credentialing process.
Links to various non-Aetna sites are provided for your convenience only. Aetna Inc. and its affiliates are not responsible or liable for the content, accuracy or privacy practices of linked sites, or for products or services described on these sites.
Changehealth.gov
Speak with a Licensed Insurance Agent 877-388-0596 - TTY 711 (M-F 8am-9pm, Sat 9am-8pm EST)
Does Medicare Supplement Plan G Cover Foreign Travel?
Eligibility for Original Medicare is an important milestone for seniors, but it may be disappointing to learn that it does not cover everything. Part A helps with inpatient care in a hospital, skilled nursing unit and religious nonmedical health care facility. Part B provides for outpatient care, medical office visits, home health services, durable medical equipment and mental health services. But both Parts A and B have a deductible, coinsurance, copayments and no ceiling on the amount of out-of-pocket expenses that may be incurred.
Some Medicare recipients choose to enroll in a Medicare Advantage plan instead, which provides Parts A and B, and often includes drug coverage and other additional benefits as well. Others prefer to stay on Original Medicare and simply want to supplement it to fill some of the gaps in coverage. The solution is often a Medicare Supplement, or Medigap, which is supplemental insurance for a series of plans labeled with letters A through N.
Asking the Right Questions When researching supplement plans, there are a few key questions that may expedite the selection process:
- How much is the monthly premium?
- What is the premium based on; for example, health status, gender, smoking history or marital status?
- Does everyone pay the same premium regardless of age, or will premium increases be imposed as I age?
- Will pre-existing conditions impact the timing of my eligibility to join certain plans?
Medicare Supplement Plan G Plan G is known for its robust coverage compared to other supplement policies. It covers all the components available in a Medigap program except the Medicare Part B deductible, and there is no limit on out-of-pocket expenses. The Part B deductible is not worth any consideration at this point because that benefit will become obsolete in 2020. The only supplement plans that currently cover it are Plans C and F, which are being phased out in 2020. Of course, the price tag reflects this suite of provisions.
Plan G is also one of the Medigap plans that include foreign travel. With so many people on the move these days, this benefit is a priority for those who travel for work or leisure. Foreign travel emergency care is covered if it begins during the first 60 days of the excursion. After meeting a deductible, the benefit amounts to 80% of the charges invoiced for specific medically necessary emergency care outside the United States. In 2019, the deductible is $250 and the lifetime limit is $50,000.
Related articles:
Does Medicare Supplement Cover Deductibles? (Opens in a new browser tab)
How Do I Choose the Medicare Advantage Plan That’s Best for Me? (Opens in a new browser tab)
Medicare Advantage and Part D plans and benefits offered by the following carriers: Aetna Medicare, Anthem Blue Cross Blue Shield, Anthem Blue Cross, Aspire Health Plan, Cigna Healthcare, Dean Health Plan, Devoted Health, Florida Blue Medicare, GlobalHealth, Health Care Service Corporation, Healthy Blue, Humana, Molina Healthcare, Mutual of Omaha, Premera Blue Cross, Medica Central Health Plan, SCAN Health Plan, Scott and White Health Plan now part of Baylor Scott & White Health, Simply, UnitedHealthcare®, Wellcare, WellPoint
Need A Medicare Advantage Quote?
Request A Free Consultation For Medicare Advantage Plans
- Credit cards
- View all credit cards
- Banking guide
- Loans guide
- Insurance guide
- Personal finance
- View all personal finance
- Small business
- Small business guide
- View all taxes
You’re our first priority. Every time.
We believe everyone should be able to make financial decisions with confidence. And while our site doesn’t feature every company or financial product available on the market, we’re proud that the guidance we offer, the information we provide and the tools we create are objective, independent, straightforward — and free.
So how do we make money? Our partners compensate us. This may influence which products we review and write about (and where those products appear on the site), but it in no way affects our recommendations or advice, which are grounded in thousands of hours of research. Our partners cannot pay us to guarantee favorable reviews of their products or services. Here is a list of our partners .
Does Medicare Cover International Travel?

Many or all of the products featured here are from our partners who compensate us. This influences which products we write about and where and how the product appears on a page. However, this does not influence our evaluations. Our opinions are our own. Here is a list of our partners and here's how we make money .
Medicare doesn’t typically cover you when you travel internationally, although there are limited circumstances when Medicare will pay for your health care outside the United States. Medicare Advantage international coverage is similar, although it differs from Original Medicare for travel within the U.S.
Be sure to confirm your travel coverage before you take flight. Here’s what you should know.
Shopping for Medicare plans? We have you covered.
Does medicare cover international travel.
Outside the U.S., Medicare usually doesn't cover health care unless [0] Centers for Medicare & Medicaid Services . Travel outside the U.S. . Accessed Aug 8, 2023. View all sources :
A medical emergency occurs in the U.S., but a foreign hospital is closer than the nearest U.S. hospital that can help.
A medical emergency occurs while you’re traveling between Alaska and another U.S. state by way of Canada, and the Canadian hospital is closer than the nearest U.S. hospital that can help.
You live in the U.S., and a foreign hospital is closer than the nearest U.S. hospital that can help. (In this case, it doesn’t have to be an emergency.)
You receive medically necessary health care on a ship within territorial waters near the U.S. (But if the ship is more than six hours from a U.S. port, Medicare won’t cover it.)
Under all circumstances, Medicare drug plans won’t cover prescription drugs purchased outside the U.S.
If you have Original Medicare and you’re traveling within the 50 states, Washington, D.C., Puerto Rico, the U.S. Virgin Islands, Guam, American Samoa or the Northern Mariana Islands, you’re covered for care from any provider that accepts Medicare.
If your health care services outside the U.S. are covered, you’ll be responsible for your normal Medicare Part A and Part B deductibles, along with any copayment or coinsurance. Foreign hospitals won’t submit a claim to Medicare for you — you’ll need to get itemized bills and submit them.
Does Medicare Advantage cover international travel?
Medicare Advantage plans , or Medicare Part C plans, provide the same coverage that Original Medicare offers, so the scenarios listed above for international travel are also true for these plans [0] Centers for Medicare & Medicaid Services . Medicare Advantage Plans cover all Medicare services . Accessed Aug 8, 2023. View all sources . Some Medicare Advantage plans may also offer emergency coverage for foreign travel. Call your plan provider for more information.
If traveling within the U.S., Medicare Advantage plans insure emergency medical care [0] Centers for Medicare & Medicaid Services . Understanding Medicare Advantage Plans . Accessed Aug 8, 2023. View all sources . Beyond that, your coverage depends on your service area and the type of plan.
Medicare Advantage plans include a network of providers, and some plans (such as HMOs ) are more restrictive about out-of-network services, so you’ll pay more for out-of-network care. Other plans (such as PPOs or private fee-for-service plans) are more flexible, although you’ll probably still pay more for out-of-network health care.
If you travel regularly and for long periods — maybe you winter in a sunny spot each year or you own a ski condo in the mountains — some Medicare Advantage plans offer “visitor” or “travel” programs for coverage while you’re away. This is something to consider, since if a Medicare Advantage enrollee remains outside their plan’s service area for more than six months, they may be involuntarily disenrolled from the plan.
UnitedHealthcare, for instance, offers a Passport feature on some plans that allows members to receive care from participating providers away from home for up to nine consecutive months.
Medicare Advantage companies
Get more information below about some of the major Medicare Advantage companies. These insurance companies offer plans in most states. The plans you can choose from will depend on your ZIP code and county.
AARP Medicare Advantage plans .
Aetna Medicare Advantage plans .
Anthem Medicare Advantage plans .
Blue Cross Blue Shield Medicare Advantage plans .
Cigna Medicare Advantage plans .
Humana Medicare Advantage plans .
Kaiser Permanente Medicare Advantage plans .
UnitedHealthcare Medicare Advantage plans .
Wellcare Medicare Advantage plans .
How to cover yourself when traveling
For peace of mind, there are a few ways you can make sure you’re covered for medical care when you’re out of your policy’s service area:
Get Medigap coverage
If you have Original Medicare (or switch back to it), you may be able to purchase a Medicare Supplement Plan (or Medigap plan) that covers foreign travel emergency health care. Standard Medigap Plans C, D, F, G, M and N cover foreign travel emergency health care [0] Centers for Medicare & Medicaid Services . Medicare Coverage Outside the United States . Accessed Aug 8, 2023. View all sources . Plans E, H, I and J also provide this coverage, but they’re no longer for sale. (If you bought one of these plans before June 1, 2010, you have this coverage.)
Under Medigap, you’re covered for foreign travel emergency care if it starts during the first 60 days of your trip. The plans pay 80% of billed charges after you meet a $250 deductible, and this coverage has a lifetime limit of $50,000.
Get travel insurance
Travel medical insurance acts like health insurance when you’re away from home, although it generally doesn’t cover routine medical care. (Need a checkup? Get that at home.) This is a policy you’d use if you broke a limb, needed emergency dentistry or required a medical evacuation, for example. If you’re traveling abroad, be sure to buy a policy that covers you internationally.
Get a Medicare Advantage plan with a travel benefit
Some Medicare Advantage plans come with travel coverage, but benefits vary, so check with your plan to get details on where and when you’re covered. Find out, too, how the plan functions: Do you pay first and file a claim for reimbursement, or will you owe a normal copay? The more you know, the better prepared you’ll be.
Carry your documents
If you’re going abroad, carry your member ID card for the insurance covering you while you’re away, plus a claim form.
What Medicare covers
Medicare covers a lot of things — but not everything. Find out where Medicare stands in the following areas:
Dental care.
Hearing aids.
Shingles vaccine.
Cataract surgery.
Chiropractic care.
COVID testing and vaccines.
Home health care.
Acupuncture.
Nursing home care.
Assisted living.
Dental implants.
Mental health services.
Addiction treatment.
Ambulance services.
Got questions about Medicare and travel? Contact Medicare at medicare.gov or 800-MEDICARE (800-633-4227, TTY: 877-486-2048).
On a similar note...
Still deciding on the right carrier? Compare Medigap plans


IMAGES
COMMENTS
Monique C. has a Medicare Advantage HMO plan from Aetna that includes the Travel Advantage feature. ... are Medicare Advantage plans that offer forms of coverage for emergency care and urgent care services during foreign travel. However, coverage and rules vary, so it is important to check with the plan administrator or insurance agent to ...
Some Medicare Part C plans include a benefit covering 80% of medically necessary urgent care received abroad. The care must begin during the first 60 days of each trip, after paying a $250 annual deductible. These plans carry a lifetime maximum benefit of $50,000. Cigna and Aetna are two companies that do have plans that cover international travel.
In order for your family member to call on your behalf, you will have to fill out some forms before your trip. Call Aetna Member Services for more information. Have questions? We can help. Call us at 1-833-570-6670 (TTY: 711), between 8 AM and 8 PM, 7 days a week. Or visit AetnaMedicare.com.
Summary. Medicare Advantage plans do not usually cover medical treatment needed when traveling internationally, but sometimes, plans may include coverage for emergency care. Private insurance ...
Some Aetna plans, for example, cover emergency care anywhere in the world, including medical evacuation. You may also consider travel insurance, which can cover medical expenses as well as trip cancellation and other concerns. Simple travel medical plans can range from $40 to $80 for a week overseas. My wife once accompanied me on a two-week ...
Overview of Medicare Supplement foreign travel emergency coverage: Carries a $250 deductible. Coverage only lasts the first 60 days of your trip. Your plan pays 80% of your medical bills while out of the country. The lifetime coverage limit is $50,000. Your Medicare Supplement plan will provide foreign travel coverage if your health services ...
Claim Form for Travel Treatment Reimbursements. How to complete this form. One form must be completed for each claimant, for each travel claim. Please complete clearly in BLOCK CAPITALS. Sections 1 to 12 must be completed in full by the claimant or the main member/spouse on their behalf, if the claimant is a dependant under the age of 18.
Medigap plans cover foreign travel emergency care that begins in the first 60 days of your trip. They pay 80 percent of the billed charges for specific medically necessary emergency care you receive outside the U.S., but you must first pay a $250 deductible for the year. Medigap's foreign travel emergency coverage has a lifetime limit of $50,000.
Whether it's an Aetna Medicare Advantage, Medicare Part D, or Medicare Supplemental Medigap plan; we're here to answer your questions and get you covered today | 855-200-5690 ... Although separate from Medicare, international travel insurance pays for emergency and routine medical services outside the U.S. Each travel insurance plan is ...
These Medigap plans: Pay 80% of the billed charges for certain medically necessary emergency care outside the U.S. after you meet a $250 deductible for the year. Cover foreign travel emergency care if it begins during the first 60 days of your trip, and if Original Medicare doesn't otherwise cover the care. You can get more information about ...
Although travel plans are frequently available with medical benefit maximums as high as seven figures, that limit is often reduced to $50,000 or less for applicants over 70 years old. Travel medical insurance can be used in conjunction with other health insurance. Many travel medical insurance plans include separate medevac coverage, but it can ...
You pay 100% of the costs, in most cases. In the situations described above, you pay the part of the charge you would normally pay for covered services. This includes any medically necessary doctor and ambulance services you get in a foreign country as a part of a covered inpatient hospital stay. You also pay the coinsurance, copayments, and ...
At Aetna International, we offer more than just health insurance benefits. You can also turn to us for resources that help make navigating your time away easier on you and your family. Get started by contacting member services and ask to speak with our International Care Management team about pre-trip planning.
International health insurance for individuals. Enjoy peace of mind wherever you travel with global medical coverage. Aetna International Health Insurance. Coverage for individuals living abroad full-time. Coverage for individuals who need care in the U.S. and abroad.
Plan G is also one of the Medigap plans that include foreign travel. With so many people on the move these days, this benefit is a priority for those who travel for work or leisure. ... Medicare Advantage and Part D plans and benefits offered by the following carriers: Aetna Medicare, Anthem Blue Cross Blue Shield, Anthem Blue Cross, Aspire ...
Based on the most recent year of data and weighted by enrollment, Aetna's 2024 Medicare Advantage plans get an average rating of 3.98 stars. [5] . For comparison, the average star rating for ...
Parts A and B: Also called Original Medicare, Part A covers services for hospital stays and similar inpatient procedures. And Part B includes coverage for doctor visits and other procedures that don't require an overnight stay in the hospital. Part C: Also called Medicare Advantage, Part C is made up of plans approved by Medicare and include all the benefits of Original Medicare.
Our global safety and security assistance solution delivers around the clock intelligence designed to meet risk management needs and support globally mobile workforces. Aetna International connects eligible members to security alerts, political and natural disaster information and 24/7 access to personalized safety advice from multilingual ...
Medicare Advantage plans offer a wide variety of benefits such as dental, vision, and hearing coverage, concierge services, gym memberships and fitness benefits, and more. ... Aetna Medicare Advantage plans can save you money and help you manage your day-to-day health needs. We have plans that include these services and programs:
Medicare Advantage plans, or Medicare Part C plans, provide the same coverage that Original Medicare offers, so the scenarios listed above for international travel are also true for these plans [0 ...
Review our Medicare Supplement Insurance plans. 87% of Aetna® Medicare Advantage members are in 4-star plans or higher for 2024. Every year, Medicare evaluates plans based on a 5-star rating system. Read the latest press release on our Star Ratings for 2024 and our ongoing commitment to improving health outcomes for members.
Call us. Talk to a licensed agent at. 1-855-335-1407 (TTY: 711) Monday to Friday, 8 AM to 8 PM. Medicare FAQs. Get answers to common Medicare questions. Aetna offers a few different Medicare Advantage plans, including HMO-POS plans, PPO plans, and Dual Special Needs Plans (DSNP). Learn more about your Medicare Advantage plan options.
Members with Aetna Medicare Advantage (MA) and Aetna Medicare Advantage with Prescription Drug (MAPD) plans can log in or register for an account below. This includes HMO, PPO or HMO-POS plans. Through your Aetna® member account you can manage claims, view plan details and more. Log in for MA/MAPD. Register my MA/MAPD.